
SIMPLIFY HEALTHCARE PAYMENTS
The Waystar Innovation Lab™
Waystar is advancing the autonomous revenue cycle with powerful AI and automation that simplify workflows, eliminate errors, and accelerate financial performance — transforming processes for healthcare revenue cycle teams nationwide.
SPRING 2026
Waystar Innovation Showcase
Watch the Waystar Innovation Showcase and hear directly from our revenue cycle experts about the
AI-powered capabilities driving real, meaningful results across the healthcare revenue cycle.
INNOVATIONS TO OVERCOME RCM CHALLENGES
Financial Clearance
Speak to an expert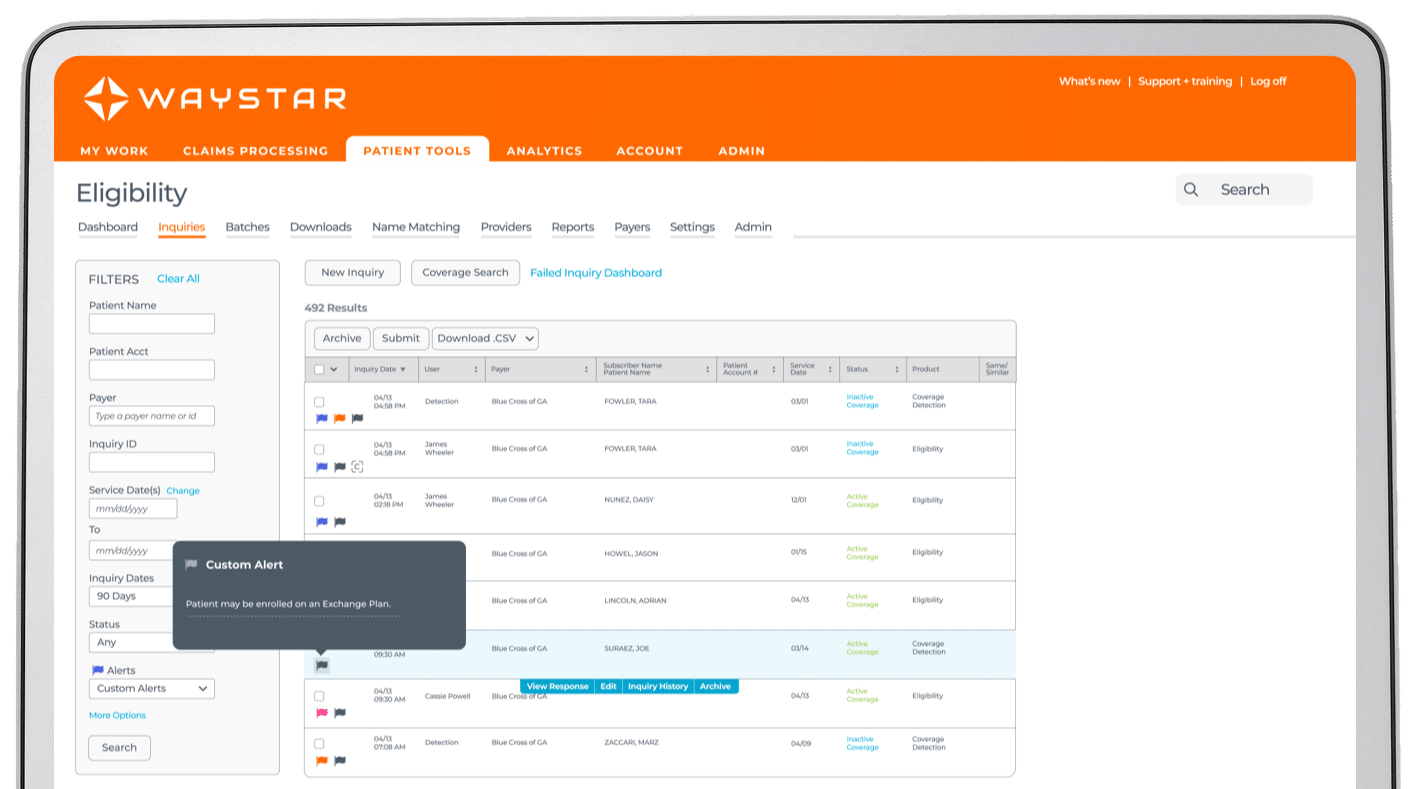
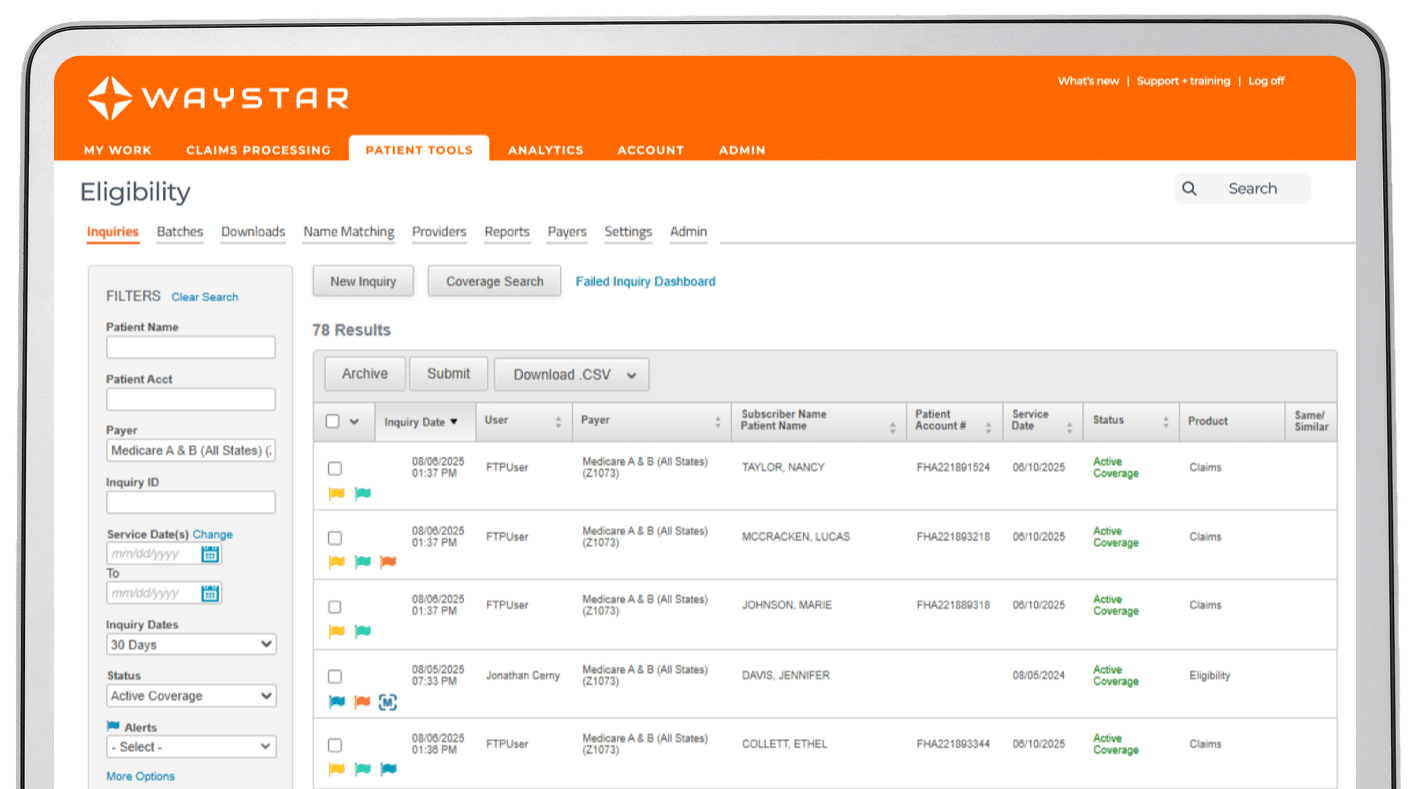
44M
authorization transactions annually
1.2K
payer connections for eligibility
30-40%
average Coverage Detection hit rate
Waystar data
Patient Financial Care
Get in touch20-30%
average collections lift
$60B
total lifetime patient payment transactions processed
35%
paper suppression rate
Waystar data
Clinical Integrity + Revenue Capture
Request a demo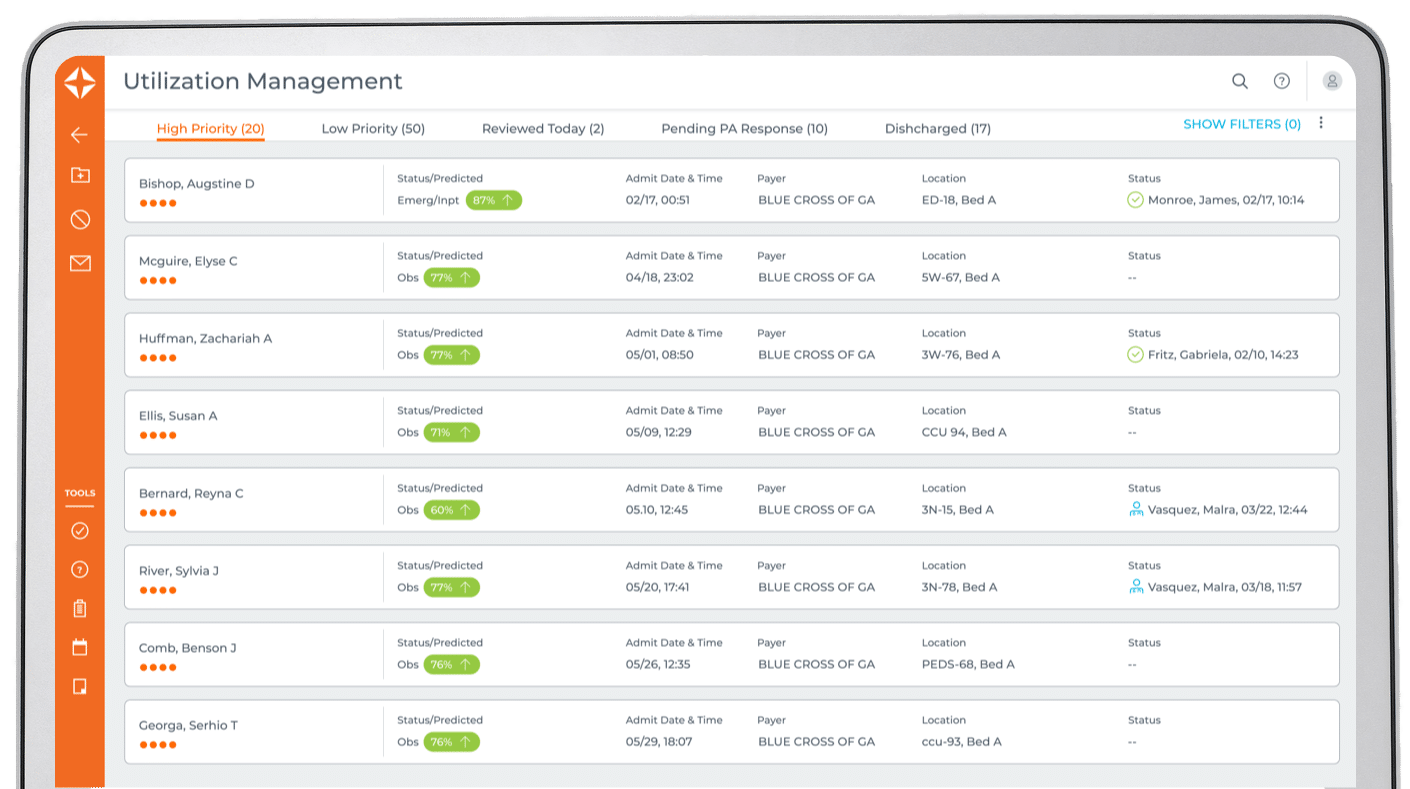
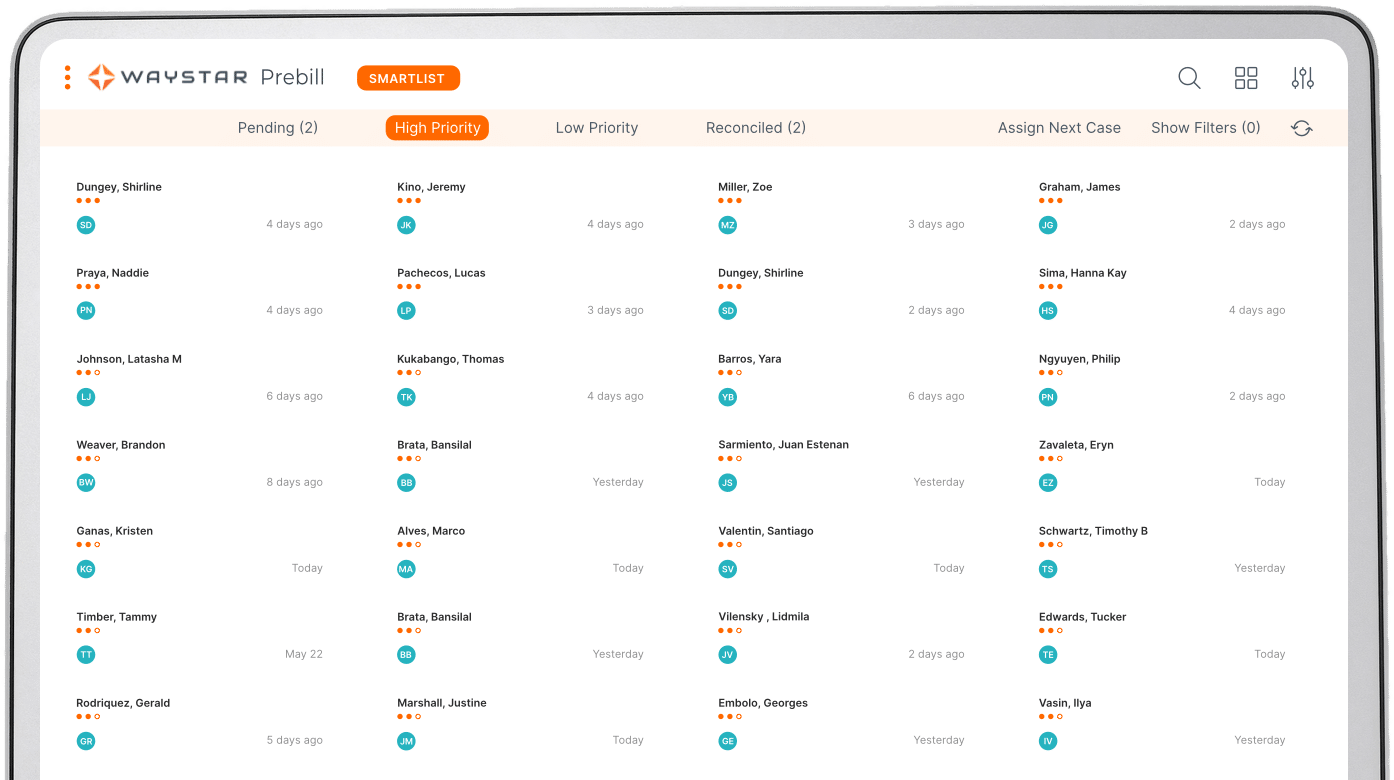
4:1
average ROI for Charge Integrity
63%
reduction in review time with Utilization Management
98%
physician response rate with Clinical Documentation Integrity
Waystar data
Claim + Payer Payment Management
Connect with an expert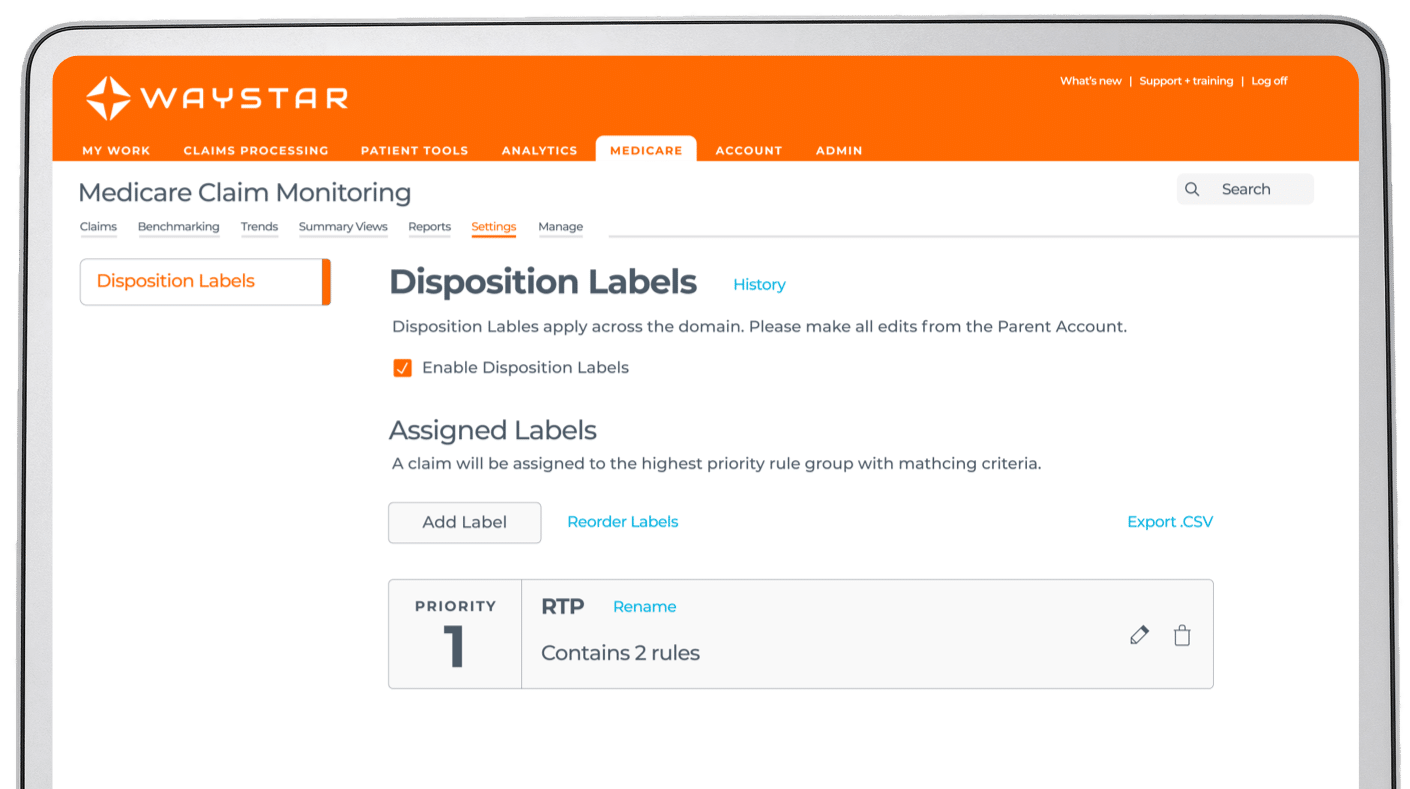

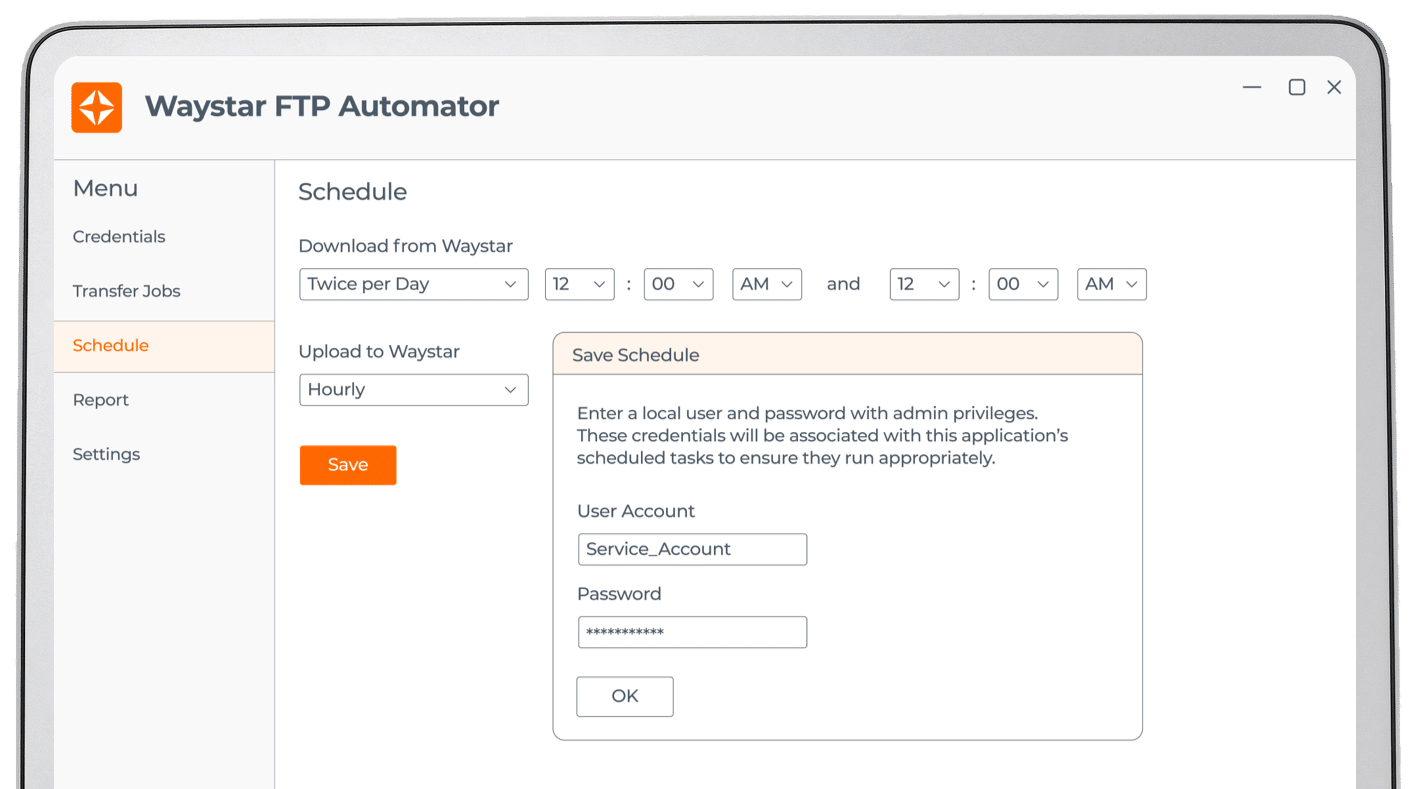
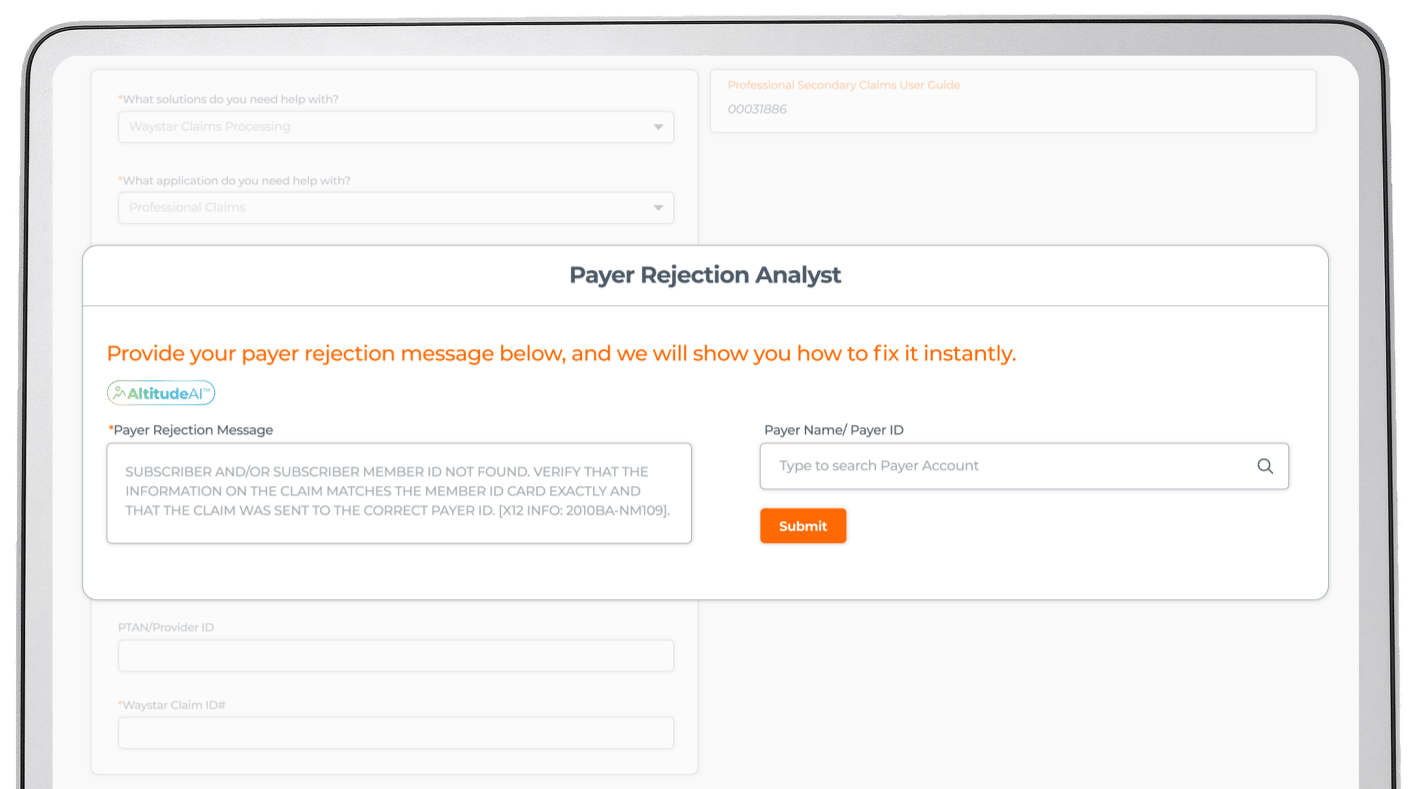
2.5M+
continuously updated edits
5K+
payer connections
98.5%
first-pass clean claim rate
Waystar data
Denial Recovery
See it in action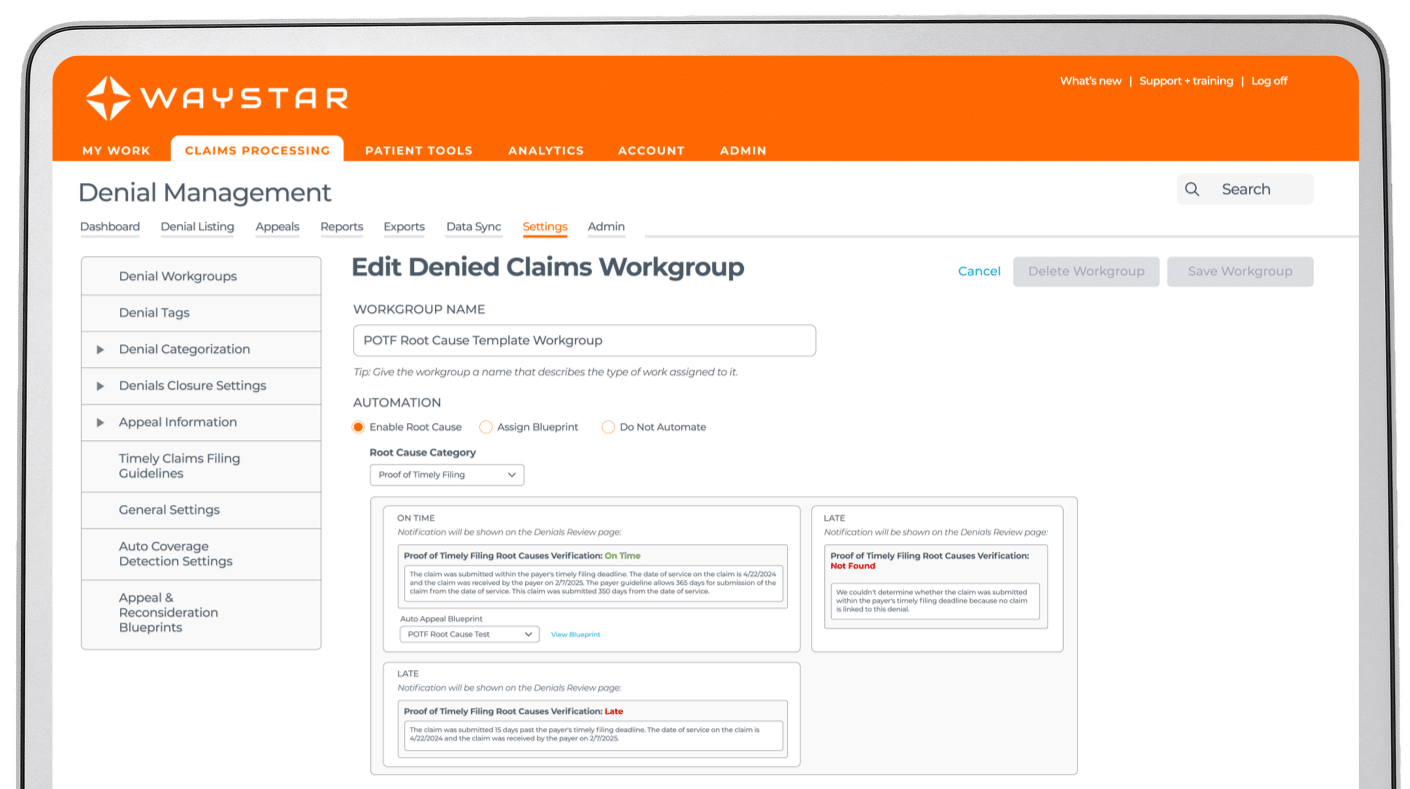

3X
faster appeal package creation with AltitudeAI™
16mins
time savings per appeal package with AltitudeAI™
86%+
recoupment to remit match rate with Recoupment Manager
Waystar data
Analytics + Reporting
Book a demo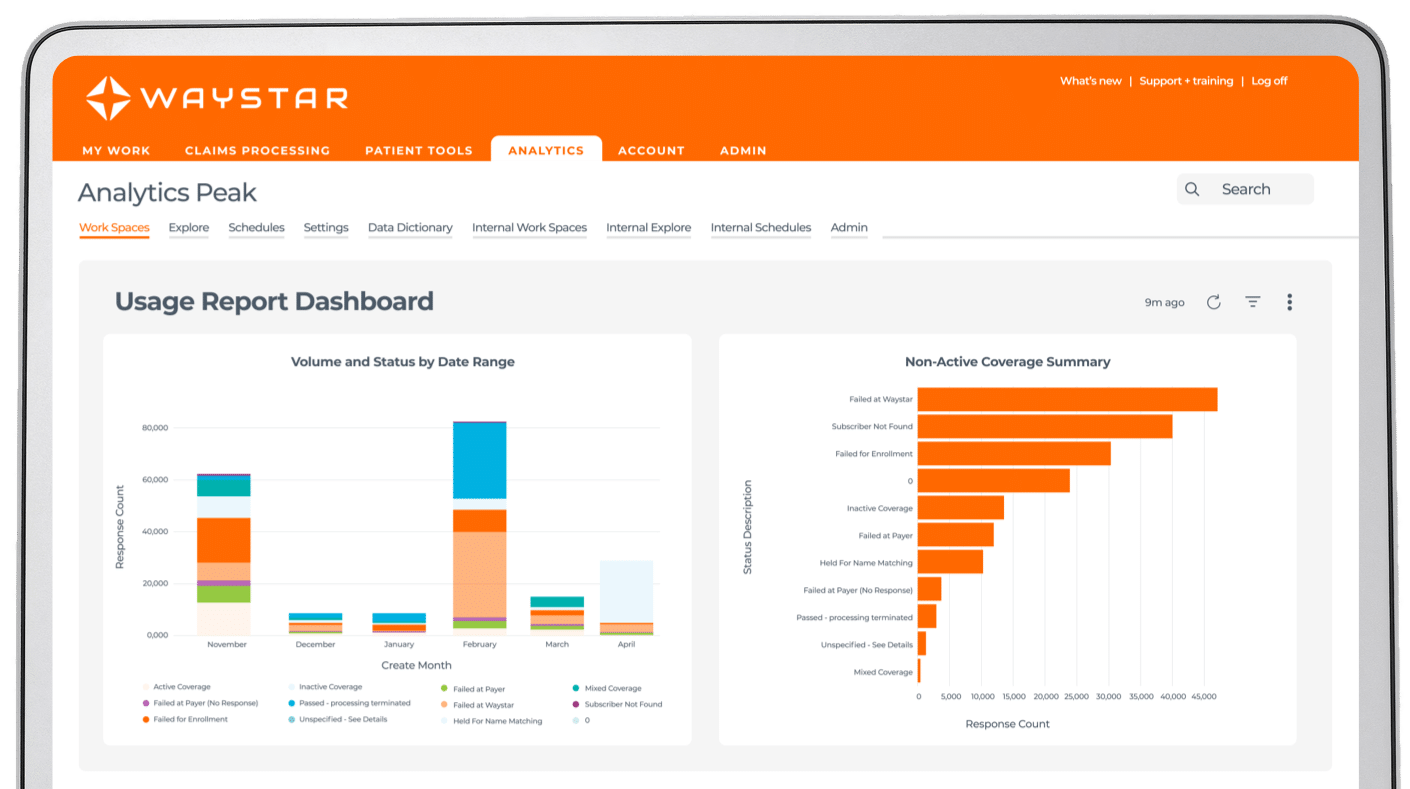

175+
pre-built KPIs for claims, remits + denials
60+
pre-built revenue cycle specific reports
12
pre-built analytics dashboards for Pro + Peak
Waystar data
LEADING THE WAY IN INNOVATION
innovation1
effectiveness1
ease of use1
1Waystar vs. Competitors, Qualtrics survey (2025)
INNOVATION IN ACTION
Trending resources

Waystar advances AI innovation with Google Cloud

Examining AI adoption + ROI in healthcare payments
Speak to a Waystar expert
Curious to learn more about Waystar’s cutting-edge innovations? Reach out to speak with a Waystar expert to learn how AI and advanced automation are helping healthcare organizations achieve meaningful results.







